HOME > Initiatives > Lifestyle Medicine
Protecting Older Adults Through Evidence-Based Clinical Practice
Falls are one of the most significant health threats facing older adults, contributing to millions of injuries, hospitalizations, and long-term complications each year.
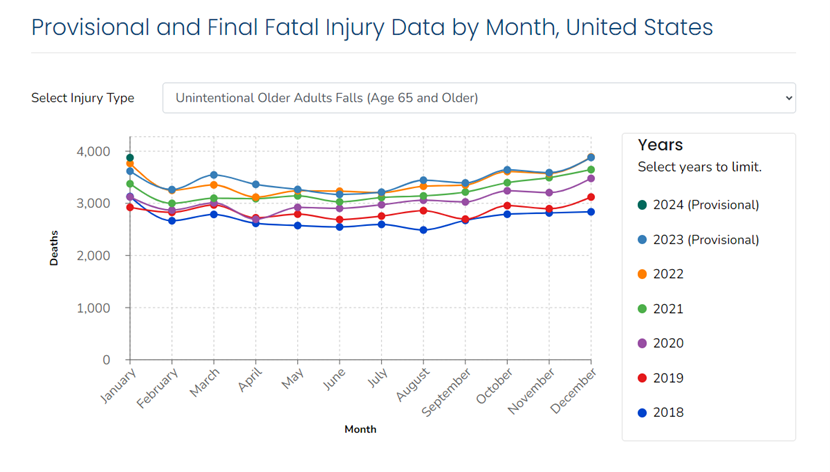
Figure 1. Provisional and final fatal fall injury data by month, United States. Source: CDC National Center for Injury Prevention and Control. This chart displays the number of older adult fall-related deaths by month and year, including the most recent provisional data available.
With funding from the Centers for Disease Control and Prevention (CDC), the American College of Preventive Medicine (ACPM), in partnership with CDC’s National Center for Injury Prevention and Control, led a national initiative to advance fall prevention in clinical practice. This effort brought together clinical leaders to develop and disseminate impactful, evidence-based tools that support providers in delivering high-quality, preventive care for older adults at risk of falls.

The Take Five for Fall Prevention infographic provides a concise, action-oriented guide for screening adults aged 65 and older for fall risk in as few as five minutes during a routine clinical visit. Grounded in the CDC STEADI framework and other evidence-based guidelines, it walks clinicians through:
Recommended interventions include medication review, physical therapy, home safety evaluation, and referral to community-based programs—making fall prevention feasible, efficient, and easily integrated into everyday clinical practice.
“Take 5 for Fall Prevention: Integrating Fall Prevention for Older Adults into the Primary Care Setting” is a webinar presented by ACPM that focuses on implementing practical fall prevention strategies in clinical settings. The webinar:
This approach recognizes that falls are a significant and preventable cause of injury and mortality in older adults. By integrating systematic fall prevention protocols into routine primary care, clinicians can substantially reduce the burden of fall-related injuries and deaths in their communities.

CDC – Older Adult Fall Prevention
National Council on Aging – Falls Prevention
USPSTF – Falls Prevention Recommendation
Key Partners and community-based organizations supporting fall prevention efforts also include Area Agencies on Aging, local health departments, and rehabilitation professionals who deliver evidence-based fall prevention programs and services for older adults.
1. Kakara R, Bergen G, Burns E, Stevens M. Nonfatal and Fatal Falls Among Adults Aged ≥65 Years—United States, 2020–2021. MMWR Morb Mortal Wkly Rep. 2023;72:938–943. DOI: 10.15585/mmwr.mm7235al.
2. Bergen G, Stevens M, Kakara R, Burns ER. Understanding Modifiable and Unmodifiable Older Adult Fall Risk Factors to Create Effective Prevention Strategies. Am J Lifestyle Med. 2021;15(6):580–589. DOI: 10.1177/1559827619880529.
3. Centers for Disease Control and Prevention, National Center for Injury Prevention and Control. Web-based Injury Statistics Query and Reporting System (WISQARS) [online]. Accessed March 11, 2024.
4. Moreland B, Legha J, Thomas K, Burns ER. Hip Fracture-related Emergency Department Visits, Hospitalizations, and Deaths by Mechanism of Injury Among Adults Aged 65 and Older, United States 2019. J Aging Health. 2023;35(5–6):345–355. DOI: 10.1177/08982643221132450.
5. Centers for Disease Control and Prevention. Surveillance Report of Traumatic Brain Injury-related Hospitalizations and Deaths by Age Group, Sex, and Mechanism of Injury—United States, 2016 and 2017. CDC, U.S. DHHS; 2021.
6. Moreland B, Kakara R, Henry A. Trends in Nonfatal Falls and Fall-Related Injuries Among Adults Aged ≥65 Years—United States, 2012–2018. MMWR Morb Mortal Wkly Rep. 2020;69(27):875–881. DOI: 10.15585/mmwr.mm6927a5.
7. Haddad Y, Shakya I, Moreland B, Kakara R, Bergen G. Injury Diagnosis and Affected Body Part for Nonfatal Fall-related Injuries in Community-dwelling Older Adults Treated in Emergency Departments. J Aging Health. 2020. DOI: 10.1177/0898264320932045.
8. Valente JH, Anderson JD, et al. Clinical Policy: Critical Issues in the Management of Adult Patients Presenting to the Emergency Department With Mild Traumatic Brain Injury. Ann Emerg Med. 2023;81(5):e63–e105. DOI: 10.1016/j.annemergmed.2023.01.014.
9. Vellas BJ, Wayne SJ, Romero LJ, Baumgartner RN, Garry PJ. Fear of falling and restriction of mobility in elderly fallers. Age Ageing. 1997;26(3):189–193. DOI: 10.1093/ageing/26.3.189.
10. Kakara RS, Lee R, Eckstrom EN. Cause-Specific Mortality Among Adults Aged ≥65 Years in the United States, 1999 Through 2020. Public Health Rep. 2023;139(1):54–58. DOI: 10.1177/00333549231155869.
11. Centers for Disease Control and Prevention, National Center for Health Statistics. National Vital Statistics System, Mortality 1999–2020. CDC WONDER Online Database; 2021. Accessed February 9, 2023.
12. Ganz DA, Latham NK. Prevention of Falls in Community-Dwelling Older Adults. N Engl J Med. 2020;382(8):734–743. DOI: 10.1056/NEJMcp1903252.
13. Centers for Disease Control and Prevention. Web-based Injury Statistics Query and Reporting System (WISQARS) [online]. Accessed 2024.
Infographic Reference
14. Gillespie LD, Robertson MC, et al. Interventions for preventing falls in older people living in the community. Cochrane Database Syst Rev. 2012;(9):CD007146. DOI: 10.1002/14651858.CD007146.pub3.
15. Johnson TM 2nd, Vincenzo JL, De Lima B, et al. Updating STEADI for Primary Care: Recommendations From the American Geriatrics Society Workgroup. J Am Geriatr Soc. Published online January 29, 2025. DOI: 10.1111/jgs.19378.
16. Montero-Odasso M, van der Velde N, Martin FC, et al. World guidelines for falls prevention and management for older adults: a global initiative. Age Ageing. 2022;51(9):afac205. DOI: 10.1093/ageing/afac205.
17. US Preventive Services Task Force. Interventions to Prevent Falls in Community-Dwelling Older Adults: USPSTF Recommendation Statement. JAMA. 2024;332(1):51–57. DOI: 10.1001/jama.2024.8481.
18. 2023 American Geriatrics Society Beers Criteria® Update Expert Panel. AGS 2023 Updated Beers Criteria® for Potentially Inappropriate Medication Use in Older Adults. J Am Geriatr Soc. 2023;71(7):2052–2081. DOI: 10.1111/jgs.18372.
19. CDC STEADI Clinical Resources. Available at: https://www.cdc.gov/steadi/hcp/clinical-resources/index.html. Accessed June 19, 2025.
20. O’Mahony D, Cherubini A, et al. STOPP/START criteria for potentially inappropriate prescribing in older people: version 3. Eur Geriatr Med. 2023;14(4):625–632. DOI: 10.1007/s41999-023-00777-y.
21. Lavan AH, Gallagher P, Parsons C, O’Mahony D. STOPPFrail: consensus validation. Age Ageing. 2017;46(4):600–607. DOI: 10.1093/ageing/afx005.
22. Seppala LJ, Petrovic M, Ryg J, et al. STOPPFall: a Delphi study by the EuGMS Task and Finish Group on Fall-Risk-Increasing Drugs. Age Ageing. 2021;50(4):1189–1199. DOI: 10.1093/ageing/afaa249.
23. Fracture Risk Assessment (FRAX). Available at: https://frax.shef.ac.uk/FRAX/. Accessed June 19, 2025.
24. Kroenke K, Spitzer RL, Williams JB. The Patient Health Questionnaire-2: validity of a two-item depression screener. Med Care. 2003;41(11):1284–1292. DOI: 10.1097/01.MLR.0000093487.78664.3C.
25. Sheikh JI, Yesavage JA. Geriatric Depression Scale (GDS): Recent evidence and development of a shorter version. Clin Gerontologist. 1986;5:165–173.
Image Credits
Clinical images adapted from: Eckstrom, E., Parker, E. M., Shakya, I., & Lee, R. (2021). Coordinated Care Plan to Prevent Older Adult Falls. National Center for Injury Prevention and Control, CDC. https://www.cdc.gov/steadi/pdf/Steadi-Coordinated-Care-Plan.pdf
ACPM is proud to provide high quality educational opportunities and interactive events for our members. Join us and consider contributing to our cause to improve communities through preventive medicine! For questions or assistance with any program or event, contact us at info@acpm.org or give us a call at (202) 466-2044.